What is it?
Flat feet is a term often used to describe feet that are hypermobile or roll in excessively. When your feet “roll in” excessively during stance, this gives the appearance that there is a loss of arch contour of the foot. This however is a misnomer… most feet when studied in the sitting position have an arch. Only during weight bearing do they collapse, hence these feet are said to be compensating for a particular condition and are displaying a movement called PRONATION – they are not really flat at all. The arch is present but, it collapses during weight bearing.
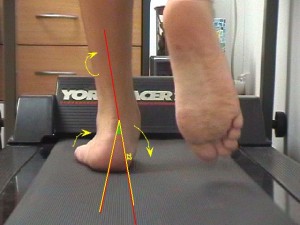
What causes flat feet?
There are many causes of abnormal pronation, the most common being:
- Hypermobility is one of the most common causes. This is present in approximately 10% of the population.
- Hereditary bony or soft tissue conditions within the foot that disrupt normal walking patterns. This causes the foot to “unlock” allowing the arch to fall closer to the ground.
- Abnormal muscle length or weak muscles.
- Abnormal leg rotations
- Poor pelvic alignment causing leg length difference
- Spinal conditions (e.g. Scoliosis)
- Muscle spasticity (e.g. Cerebral Palsy)
The result of pronation can vary from patient to patient but it should be noted that this abnormal force on the body is a major contributor of a myriad of bony and soft tissue problems; often leading to pain!
When flat feet or pronation forces become excessive or abnormal, symptoms may occur in the following areas:
- Feet (e.g. bunions, hammer toes, corns, calluses)
- Heels (e.g. plantar fasciitis, heel spurs, heel pain, Sever’s disease)
- Shins (e.g. shin splints, posterior tibial tendinopathy, PTTD)
- Knees (e.g. patellofemoral syndrome, chondromalacia (runners knee), Osgood Schlatter’s disease
- Thighs (e.g. Iliotibial band syndrome)
- Hips (e.g. greater trochanter bursitis)
- Upper and lower back (e.g. sciatica, disc protrusion)
- Neck and head secondary to poor postural alignment which can occur with kyphosis.
How is it treated?
Your Podiatrist will carry out a detailed biomechanical assessment of your feet, legs, knees and hips to identify the cause.
An analysis of your walking pattern utilising computerised video gait analysis software is performed to assess the affect on your gait. Your Podiatrist will then discuss your treatment options which will often include a pair of orthotic appliances to control any abnormal forces causing any associated foot pain, leg pain or other symptoms.
A computerised 3D LASER scan is taken of your feet and a detailed prescription is devised for you from which a pair of orthotics can be made. A prescription orthotic device is then produced which fits inside your footwear.
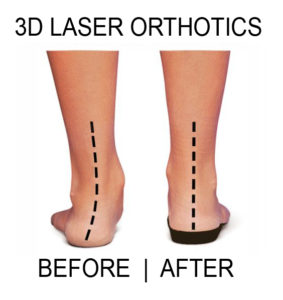
Obviously different conditions will require specific therapy. This may involve exercises, mobilisation, manipulation, massage, footwear advice, postural balance programs, dry needling or, in some cases, radial shock wave therapy. All of these options will be discussed with your Podiatrist if they feel you require this treatment.
Call Podiatry Care or book online to discuss how we can help you make your next step PAIN FREE.


